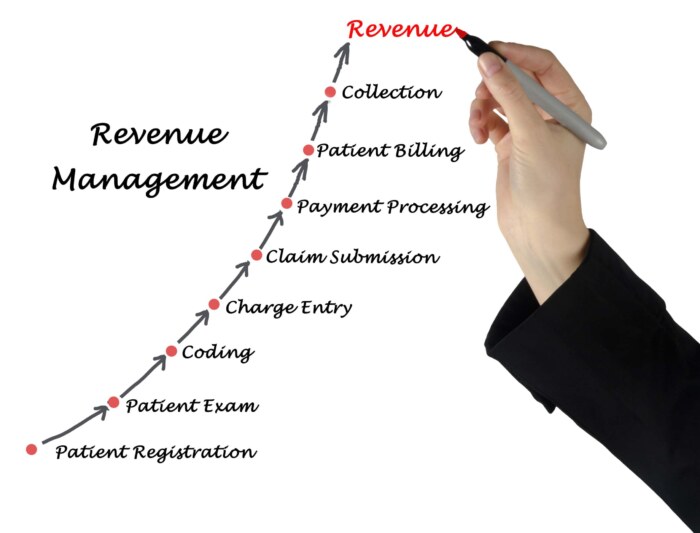
What Is Healthcare Revenue Cycle Management?
Hospitals and other healthcare facilities have a primary focus of helping patients access medical care, but this care needs to include functions and processes that allow it to be funded sustainably, and that’s where healthcare revenue cycle management (RCM) comes into play.
Without suitable financial planning, facilities would struggle to maintain patient care and continue with day-to-day operations. Revenue cycle management allows them to collect fees and keep up with any expenses to maintain a high level of care and keep on top of necessary administrative tasks.
What is Healthcare Revenue Cycle Management?
In its most simple form, healthcare revenue cycle management (RCM) is the process used by facilities to track the entire process of attaining revenue from patients for treatments and services from the very first appointment right up until the final payment of the total balance.
As described by the Healthcare Financial Management Association (HFMA), the revenue cycle includes any administrative functions as well as any other functions that “contribute to the capture, management, and collection of patient service revenue.” – The cycle essentially follows the patient through the entire process from the first encounter until final payment.
A typical cycle will include the following functions:
- Charge capture: Calculating medical services and converting them to billable charges.
- Claim submission: This involves the submission of any claims and fees to relevant insurance companies.
- Coding: All patient files will be matched with ICD-10 codes that indicate diagnosis.
- Patient collections: Determining patient balances and collecting payments.
- Pre-registration: Pre-registration can be absolutely key to optimizing RCM. Collected preregistration information can include patient details and insurance coverage before a patient arrives. This can identify other requirements such as if a patient will require a Good Faith Estimate.
- Registration: Establishing a medical record number by gathering further patient information and meeting necessary regulatory and financial requirements.
- Remittance processing: Applying or rejecting payments through remittance processing.
- Third-party follow up: Collecting payments from third-party insurers.
- Utilization review: This focuses on the necessity of the treatments and medical services.
Why is Revenue Cycle Management Important?
Healthcare revenue cycle management is vital to any medical facility. Of course, their primary aim is to save lives and help patients, but without the necessary funds to do so, the quality of care begins to decline and both patients and healthcare professionals see the effect of this.
Revenue cycle management is about ensuring that revenue within facilities is properly managed and contributes to the cyclical maintenance of the facility and services within the facility and beyond.
Challenges Addressed by Healthcare RCM
Collecting Patient Payments
Collecting payment from patients has never been a simple task, regardless of whether collections are made before or during treatment. This is one reason why efficient RCM is so key to the continued success of treatment.
Due to high premiums and financial hardships, many patients are unable to pay medical costs in full and upfront. Healthcare facilities must strike a compromise between timely payment collection and avoiding losing patients altogether. Some providers, for example, have improved patient payment choices. Other providers have given patients the option of extending payment terms or deferring payments, or provided payment plans that better suit patients. RCM helps facilities to keep track of all of this information.
Internal Errors
At the end of the day, employees are people and even the most knowledgeable and experienced people make mistakes. But what can be done to reduce the impact that human error has on the financial management of an institution?
Regular employee education programs that promote accurate coding practices, detailed chart documentation, and financial policy reminders should be actioned by healthcare institutions. Regular and easily implemented training sessions have been proven to minimize significant errors in processes and in things like charge capture and patient information gathering.
Of course, there is always an argument for automating these processes where possible. Not only will it save significant time but with the correct data and systems in place, much of the manual processing can be removed and with it, room for small administrative errors that are sometimes missed.
Authorization Barriers and the No Surprises Act
Prior permission processing can also make revenue cycle management difficult for facilities. Prior authorization regulations force providers and their patients to wait for the health plan to approve a service before receiving or providing it. The No Surprises Act particularly has been a cause for concern for revenue cycle management executives, with additional legislative changes adding even more complexity to collecting payment. The No Surprises Act prohibits out-of-network doctors from billing consumers for more than their in-network cost-sharing level. The policy itself is excellent for protecting patients from unexpected bills, but it has caused more headaches for IT teams and those in charge of optimizing internal processing.
Facilities must alter their revenue cycle procedures to comply with the No Surprises Act, which went into effect on January 1, 2022.
How Can You Optimize Revenue Cycle Management?
Transparency With Charges
One of the most simple ways to optimize revenue cycle management is to prioritize transparency. With new legislation like the No Surprises Act and the Good Faith Estimate ruling, facilities are already having to be very open with patients about costs, but it can really work to your advantage.
The whole purpose of revenue cycle management is to create a process that focuses on obtaining patient service revenue, and there’s no better way to ensure prompt payment that to provide patients with clear information on costs so that they can prepare for those charges rather than avoiding payment, or even worse, going to a different, more cost-effective facility.
Providing costs up front not only allows patients to identify whether they can afford services, but it gives them an opportunity to source financial support should they need it. This preparedness can only help a facility when it comes to billing and collecting payment.
Data and Analytics for RCM
To get a comprehensive view of the revenue cycle, facilities should use data and analytics.
In the wider business world, data and analytics are essential, and for financial management they can be even more key. For better healthcare revenue cycle management, dashboards and robust reporting are recommended and there are numerous systems i3solutions can help you manage your data and link your software together for a more comprehensive view.
Measurements and data analytics will be required to better manage the revenue cycle and identify any problem areas. Monitoring KPIs to track the revenue cycle’s health is also a critical element of this, made much more simple with clear and concise analytics systems.
Healthcare Revenue Cycle Management Systems
There are a number of prominent vendors selling either stand-alone RCM products, or systems integrated with Electronic Health Record systems. Here are just a few options:
- McKesson – McKesson is a major supplier of pharmaceuticals, medical supplies, and health IT products and services.
- Meditech – Meditech sells health information technology to over 2000 healthcare facilities across North America, and the UK.
- Epic Systems – Epic Systems is a major provider of health IT systems, mostly to large U.S. hospitals to help with accessing, organizing, storing, and sharing patient medical records.
- Cerner – Cerner is a health information technology company.
- Athenahealth – Athenahealth is a cloud-based practice management system provider for small to medium-sized medical facilities.
Many facilities already have intricate RCM systems like these in place to try and cope with the huge task of managing financial processes in a constantly changing healthcare industry. Maintaining policies and keeping processes uniform throughout a facility can be a challenge, which is where properly integrated systems can be a huge benefit. i3solutions can go a long way in assisting with this.
How to Improve Healthcare Revenue Cycle Management With Technology
Automation is an absolute game changer for many healthcare facilities. It’s often overlooked because companies can often find it hard to trust IT to handle what have historically been manual tasks. But technology has advanced to the point where properly integrated computer systems can actually work much more efficiently at some tasks than people and provide facilities with more time to focus on essential healthcare.
A company like i3solutions, with over 25 years of experience helping businesses and healthcare facilities make the most of their systems, can manage installs and help to connect the dots to make all of your data and systems work together seamlessly. If this sounds like something you could use some assistance with, then you can get in touch to discuss your options.
Leave a Comment